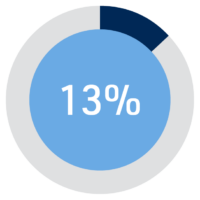
The average percentage of expired-product waste in the operating room (OR) is 13%, according to the results of a new survey of Perioperative leaders conducted by the Association of periOperative Registered Nurses (AORN) and commissioned by Owens & Minor.
While on the surface that percentage seems like a drop in the bucket when considering overall Perioperative supply costs, this finding offers a critical insight into a major patient safety issue facing OR teams today.
If operating rooms have in their inventory an average of 13% of products that expire on the shelves, what is the risk of a clinician using an expired product on a patient? Consider how Perioperative supply inventory includes not only general medical/surgical supplies but also high-cost, high-risk consignment products, such as implants and stents, and the stakes become clear.
This leads to the question: If OR teams cannot track product expiry with current systems, what capabilities are they lacking and how can technology and solutions providers fill that gap?
The OR’s inventory management problem
When asked about specific challenges in their ORs, 62% of Perioperative leaders surveyed rated supply related factors as “very” or “extremely” problematic, with 20% reporting challenges documenting product usage in patient care.
While operating rooms have implemented technology solutions to help drive efficiency across many of their processes, they still handle 40% of them with manual intervention, specifically those related to supply management. Only 21% of OR leaders surveyed say they use barcode scanning to document materials used in a procedure, while 70% report using manual data entry.
Another significant problem reported by Perioperative leaders is physician preference card management, which was cited as the top reason supplies are picked for a case but not used (40% of respondents). Only 7% of survey respondents report their cards as mostly accurate.
The big picture on patient safety
If OR teams cannot effectively manage their supply inventory, or document item usage in procedures, how do they know if they have expired items on their shelves? More importantly, how do they prevent expired products from entering the OR and being used on a patient?
Furthermore, physician preference card inaccuracies lead to a high percentage of items that are picked but go unused and must be returned to inventory. As supplies make their trip from defined storage areas to the OR and back again, there is the risk they will be lost along the way. Perhaps a nurse decides to keep some items in the OR as “just in case” inventory in the event they are needed.
If supplies circulate around the Perioperative setting without oversight from supply chain, there is a greater risk that expired products could remain in inventory, and therefore a higher chance they will be used.
Gain visibility and control
Owens & Minor’s QSight® is an end-to-end, cloud-based perpetual inventory management system that facilitates automated point of use (POU) product data capture and physician preference card management with full integration to the hospital’s materials management information system (MMIS) and electronic health record/electronic medical record (EHR/EMR).
With QSight®, the OR team has real-time visibility into supply inventory and can closely track what items are picked, used, returned, and wasted. The QSight® solution continually updates inventory counts and delivers actionable data to Perioperative leaders so they can make effective, informed supply decisions.
Leveraging AI driven insights, QSight enables OR teams to set up custom alerts notifying them of when products are set to expire (e.g., 30, 60 days ahead of time). With this visibility and knowledge, the team can optimize inventory by using items ahead of their expiry dates, even moving them from one OR to another based on supply levels and case schedules.
Most importantly, it helps an OR team avoid “never events” that could lead to patient harm. In addition to expiry tracking, the solution matches supply inventory to recalled items, and alerts a clinician if they attempt to use an expired or recalled product on a patient.
Looking For More Of The Latest Trends In Operating Room Efficiency
The 2023 Owens & Minor Operating Room Efficiency Research Report presents key findings from the survey of 250 perioperative leaders. This report offers quantitative insights into how efficiency in an operating room correlates to patient outcomes and drills down into specific factors that generate unnecessary labor costs and waste.