Healthcare is a complex subject and one that requires constant attention to maintain patient and healthcare provider safety. The risks for Healthcare-Associated Infections (HAIs) are a real and present danger for patients across the entire healthcare continuum of care.
Over the past few years, the role of the clinical environment of care has been better understood, medical devices complexity has steadily increased, and the comorbidities of patients continue to pose unique challenges in terms of infection control efforts. In response to the ever-changing threats associated with HAI transmission, the Centers for Disease Control and Prevention (CDC) developed the new Core Infection Prevention and Control Practices for Safe Healthcare Delivery in All Settings. These new recommendations were released by the CDC Healthcare Infection Control Practices Advisory Committee (HICPAC) in an effort to help hardwire the most critical elements of infection prevention and control so that every single patient is protected from the risks of HAIs regardless of the clinical care setting.
The CDC Core Practices recommendations include the following key elements:
1. Effective Leadership and Support
Infection Prevention and Control starts and ends with the Chief Executive Officer (CEO). Leadership must resource the program which may include personnel, technology, or program resources. Active leadership involvement is critical to the long-term success of any infection control program
2. Education and Training of Healthcare Personnel on Infection Prevention
Education must extend beyond basic training techniques and focus on role-specific competency. This competency-driven approach assists healthcare staff members with safely performing their role.
3. Patient, Family, and Caregiver Education
Education goes well beyond the healthcare team and extends to both families and caregivers, especially in outpatient settings such as home care.
4. Performance Monitoring and Feedback
Infection Control practices must be continuously assessed in order to monitor for compliance. If infection control practices are not being properly followed, clinicians must be afforded immediate constructive feedback specific to improvement strategies.
a. Hand Hygiene
Hand Hygiene remains the single most important infection control intervention that we have in our toolkit against infectious diseases. The regular practice of hand hygiene with either soap and water or an alcohol-based hand rub can help stop the transmission of germs in their tracks. Our goal must be 100% hand hygiene for not only the healthcare team, but also our patients.
b. Environmental Cleaning and Disinfection
The use of an EPA-registered, broad-spectrum disinfectant on potentially contaminated environmental surfaces will remove bioburden and potential microbes from the clinical environment of care. In today’s COVID-19 era, it is also important to utilize an EPA-registered disinfectant that is found on the EPA List N, which indicates effectiveness against SARS-CoV-2, the virus that causes COVID-19 infection.
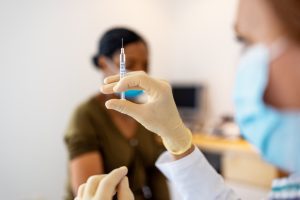
c. Injection and Medication Safety
The reuse of needles and syringes continues to plague our healthcare system, especially in some outpatient settings. Healthcare professionals must carefully follow the manufacturer’s instructions for use for single-use and disposable injection devices to prevent potential transmission of bloodborne pathogens.
d. Risk Assessment with Appropriate Use of Personal Protective Equipment
While Personal Protective Equipment (PPE) is routinely used in healthcare to stop the spread of infectious diseases, PPE is the last line of defense in transmission. Other measures such as Engineering Controls should serve as the primary mode of intervention.
e. Minimizing Potential Exposures
Healthcare professionals should avoid unnecessary exposures to infectious diseases and use only the core personnel necessary to safely deliver clinical care.
f. Reprocessing of Reusable Medical Equipment
Medical equipment should be cleaned, disinfected, and reprocessed according to the manufacturer’s instructions for use. This may include a range of reprocessing options from low-level disinfection with an EPA-registered disinfectant to sterilization.
5. Transmission-Based Precautions
Transmission-based precautions focus on infection control interventions centered on the pathogen’s route of transmission.
6. Temporary Invasive Medical Devices for Clinical Management
Early and prompt removal of invasive devices should be part of the plan of care and included in regular assessment. Healthcare personnel should be knowledgeable regarding risks of the device and infection prevention interventions associated with the individual device and should advocate for the patient by working toward removal of the device as soon as possible.
7. Occupational Health
Every day, protecting the health and wellness of healthcare workers is a crucial aspect of the infection prevention program. Healthcare workers must stay home when sick and the healthcare employer must support these employees who refrain from actively working while ill.
Regardless of the pathogen of concern, these infection prevention control practices reduce risks, improve clinical outcomes, and decrease overall healthcare costs. COVID-19 has changed the dynamics of our healthcare system, and now more than ever, we must take all necessary steps to ensure the safety of both our patients and also our colleagues. Adherence to these core practices is an important aspect in maintaining patient safety and also preventing the spread of potentially infectious diseases in both healthcare and community settings.
References
Core Infection Prevention and Control Practices for Safe Healthcare Delivery in All Settings, electronically accessed from: https://www.cdc.gov/hicpac/recommendations/core-practices.html, Centers for Disease Control and Prevention Healthcare Infection Control Practices Advisory Committee, 2019.
About the Author
Dr. Garrett is the President and CEO of Community Health Associates, LLC. And also has an appointment as an Adjunct Assistant Professor of Medicine in the Division of Infectious Diseases at the University of Louisville School of Medicine. Dr. Garrett is a frequent lecturer globally on patient safety, infectious diseases, and medical device reprocessing and safety.